Recently we asked Natalie van Winckel, Senior Early Parenting Sleep Consultant and Education Lead from Nourish Baby and Safe Sleep Space, to share her insights into what separates noisy babies from others who are less vocal.
Recently we asked Natalie van Winckel, Senior Early Parenting Sleep Consultant and Education Lead from Nourish Baby and Safe Sleep Space, to share her insights into what separates noisy babies from others who are less vocal.
- Babies exhibit varying levels of vocalisation, with some being louder and more vocal than others
- Babies may produce different sounds during settling, sleep, and wakefulness due to developmental stages and reflexes
- Parents can use techniques like listening and waiting, offering gentle comfort, and interpreting cries to soothe their noisy babies
- Babies go through stages of vocal development, from cooing and gurgling to babbling and speech, which may influence their sleeping patterns and noises
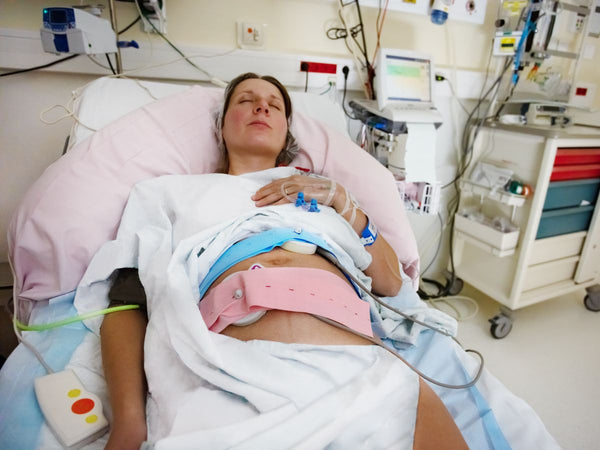
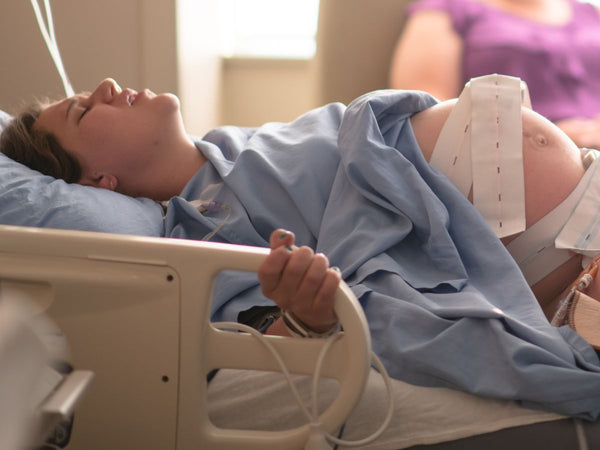
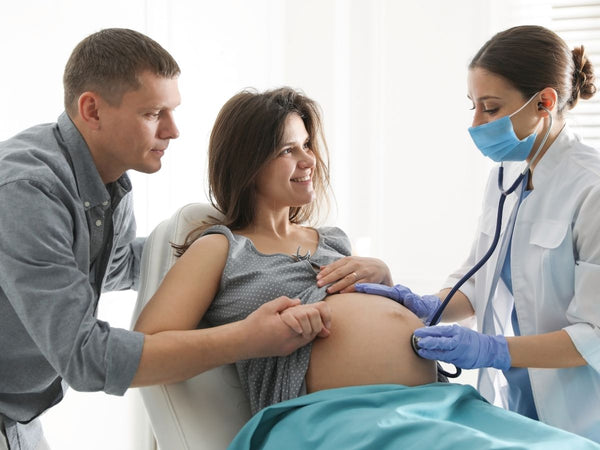
It’s true to say that some babies are more than generous in sharing with the world that they’re around. Others are happy to stay in their own little bubble, quietly cooing and babbling away to themselves. Crying, squealing and grunting are common languages for babies who don’t seem to have a volume control. If your little person is one of many who could be described as a ‘noisy baby’, welcome to the club.
Insights from a baby sleep expert
Recently we asked Natalie van Winckel, Senior Early Parenting Sleep Consultant and Education Lead from Nourish Baby and Safe Sleep Space, to share her insights into what separates noisy babies from others who are less vocal.
Natalie said that in her experience, crying during settling is often different to crying during other periods. “Crying during settling often involves more prolonged or intense vocalisations compared to typical baby noises.” “Simple or normal baby noises are often shorter and more varied, like grizzles, coos or sucking sounds.”
When it comes to newborns and young babies, Natalie explained, “They can make noises in their sleep for a few reasons, their immature gut/brain connection could be causing lots of grunting, wriggling and squirming when the baby is sleeping even though their eyes may be closed.” “Their little digestive systems are still developing and this can cause more noises associated with their digestion.” “In most cases, these noises are a very normal part of their development.”
Natalie advises parents who may be worried to take a recording of their baby when they’re sleeping and making these noises and seeking out medical advice. Our baby sleep guide provides all the information and support you need as a parent.
Sleep stages and development
Another important point which Natalie shared is that “Newborns spend a significant window, up to 75% of their sleep, in the Rapid Eye Movement (REM) Phase.”
“This kind of sleep is much lighter and they may exhibit facial twitches, eye movement and little smiles, as well as sounds or cry outs.” Babies are also born with a startle reflex, “And this can lead to startled sounds or brief wakeups if they’re exposed to sudden loud noises or movements.” “The startle reflex does diminish with age.” Natalie reported.
Swaddling can be a good strategy to help contain a young baby’s startle reflex. But it’s important to leave the baby’s arms free once their startle reflex disappears, at around 3 months of age.
Just be yourself baby
When it comes to why some babies are noisier than others, Natalie said that in her experience, “Factors such as individual temperament, developmental stages, some babies just being naturally more vocal and others being quieter” are common features. And for lots of little people “They like to make noises which help them to self soothe or wind down in preparation for their sleep, it can be very comforting for them.”
Parents can find that sometimes it’s hard to work out why a baby is crying, especially when all their needs have been met and they still seem unsettled. It’s important that parents are emotionally and physically available to help their baby soothe and settle.
It can help to get support from others and remind ourselves, parenting is often difficult. With time and gut maturity, most babies develop fairly regular patterns of feeding, sleeping and being awake. Getting to that age and stage is different for every baby.
It sounds like you’re calming
So, now we understand more about why some babies are noisier than others what can we do to comfort them when they’re making those vocal exchanges? And importantly, do we need to do anything? Again, Natalie shared the benefits of her experience, “You know your baby best.” “Often a listen and wait approach can be beneficial to see what those little noises are telling us; if they decrease from grizzling to cooing or sucking, then the baby is managing.”
“If these noises increase from grizzling to crying, then offering some voice comfort such as shshing or coming down to the side of the cot or bassinet and offering some gentle hands on comfort may be all your little one requires to settle back into a deeper sleep.” “If at any time, you’re not comfortable with your baby’s noises, go in and check on them as often as you need to.”
Some other tips about noisy babies
It can be helpful then for parents to try to interpret their baby’s cries and noises as being unique, according what they need. Just like adults, babies adjust their pitch and intensity when they’re communicating, depending on what they want to say. But interpreting individual cries and protests and decoding them is often challenging, especially for exhausted parents.
A common household scenario is that baby cries and parent quickly responds – often with the aim of supporting the baby to calm in the shortest way possible. Because hearing our baby cry, especially when we’re sleep deprived, can be particularly difficult and sometimes, intensely irritating.
You’re sounding older now!
Babies go (and grow) through different stages of vocal development. By 3 to 6 months, babies tend to become more aware of their own voice. This is the age when skills in cooing and gurgling for pleasure are developing. Babies also begin babbling and listening more intently at around 3- 4 months. These are skills which help to support their speech and language development.
Natalie added, “Whenever a baby is learning a new developmental skill, they will often go through a period of having noisier sleep.” “You will often see this when your little one is learning to coo, learning to speak new words, or when they begin to dream and (perhaps) want to recall their dream they’ve just had.”
“Around the time your baby starts solids or changes milk types, digestive issues may sound more discomforting.” Natalie recommended parents make a note of these noises and how their baby’s sleep has been over a few nights, then discussing this with their health professional to know the best way to manage.
Noisy breathing
Noisy breathing is a different matter to crying and squealing. Sometimes babies make a noise when they breathe – medically known as stridor. One of the many reasons for stridor is a condition called laryngomalacia, or ‘floppy larynx’. This is caused by the soft tissues in the baby’s larynx (voice box) being soft and floppy, most frequently from birth.
The majority of babies with laryngomalacia don’t have problems with their breathing or feeding, it’s just their breathing is noisy. By around 12 months of age, most babies have grown out of laryngomalacia.
Remember to have your baby checked by a doctor if you are worried about their breathing.
Check our blog for more interesting and informative articles or check out our range of antenatal education resources.
Written for Nourish Baby by Jane Barry, Midwife and Child Health Nurse.