Key points
- A labour induction may be offered if there is a risk to a mother and/or her baby by continuing with the pregnancy.
- There are a few ways labour can be induced. Often a combination of strategies is used.
- Induction isn’t for all women – some prefer for natural labour to start.
- After an induction it’s important to be closely monitored.
What is an induced labour?
An induced labour, also called an induction or Induction of Labour (IOL), is a process where labour is started artificially. A maternity care provider, either a midwife or obstetrician, uses techniques to mechanically dilate the cervix, break the membranes (waters) or start the contractions. Often, an induction is a combination of two or more of these procedures.
Statistically, in Australia, one in three women have their labour induced. Generally, inductions are done in hospital, though having a ‘stretch and sweep’ procedure (see below) can also happen during an antenatal appointment.
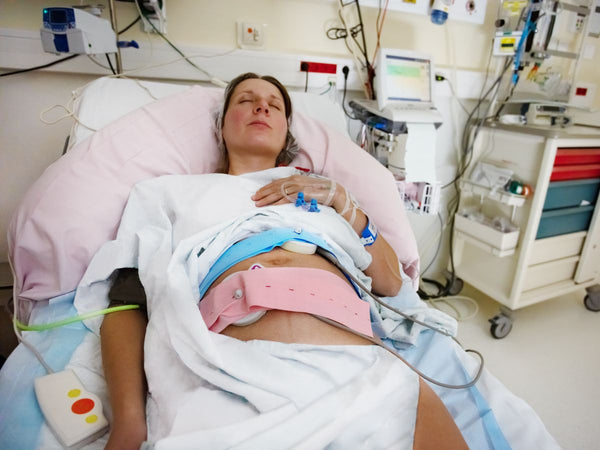
But I don’t understand why I need an induction!
It’s important that you feel fully informed and give your consent to having your labour induced. It’s also valuable for you to understand that the benefits are clear and the risks minimal. Your maternity care provider has a professional responsibility to discuss the benefits and risks of an induction.
It’s fair to expect your maternity care provider to explain why you need an induction, what the risks are of having or not having one and what may happen if you wait for your labour to start naturally. You also need to understand how your labour will be induced and what options you have.
What are the differences between an induced labour and a natural labour?
Normally, labour starts without intervention between 37-42 weeks of pregnancy. The waters break and/or, contractions start and labour progresses naturally.
Natural labour tends to be slower than an induced labour. The contractions build slowly until they become more frequent and more intense. In an induced labour, contractions can start very quickly and be strong from the start. Women who have an induced labour can feel they need pain relief earlier in their labour.
Having an induced labour increases the risk of needing further interventions. This can include having a forceps or ventouse assisted birth. Birthing women who have an induction can also have less opportunity to be mobile during their baby’s birth because the baby needs monitoring more closely.
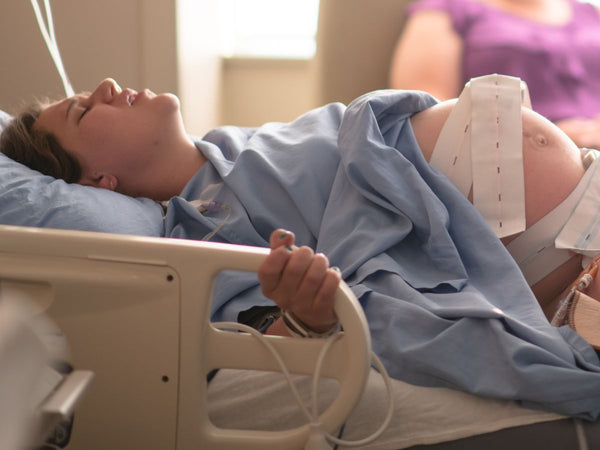
Can’t I just wait until my labour begins naturally?
As a baby’s due date approaches, nature prepares the cervix to start thinning and dilating. However, if there’s a risk to a mother’s or her baby’s health, inducing labour can be the safest option. By two weeks past the baby’s due date, the amniotic fluid can start to reduce in volume and there can be an increased risk of the baby being larger than average. There is also an increased risk of general maternal and foetal complications.
Why would I need to have my labour induced?
There are a few reasons why induction can be recommended. Generally, an induction is recommended when there are risks to a mother’s or her baby’s health by continuing with the pregnancy.
Common reasons for induction include:
- Being overdue – the pregnancy has gone more than 10-12 days over the due date.
- The placenta is not working as efficiently as it should be.
- Health conditions for a mother such as high blood pressure, kidney problems or diabetes.
- Slowing down of foetal movements and/or, an abnormal CTG (Cardiotocograph).
- Induction of labour may be appropriate within 24 hours of premature rupture of membranes if the baby has not yet been born.
- Social reasons such as a living some distance from the maternity hospital, a partner needing to go away or a maternity care provider’s availability.
- The waters have broken but contractions have not started naturally.
- Having an infection in the uterus.
- Having a multiple pregnancy.
- When there is little amniotic fluid around the baby – oligohydramnios.
- When a baby has died in the uterus or in unlikely to survive outside of the uterus.
Some women find advanced pregnancy very difficult to tolerate. In some circumstances, a woman’s request for an induction is considered if she feels her physical and mental health is being compromised by waiting until labour starts naturally.
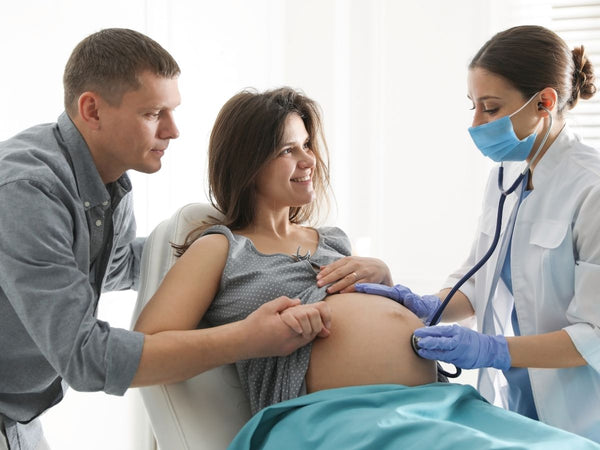
When would an induction not be recommended?
An induction of labour is not recommended for all women. Women who have had a previous caesarean section and who are induced with subsequent labours are at a higher risk of having a uterine rupture.
If the placenta is lying over the cervix, placenta praevia, or the baby is lying sideways or breech, an induction is generally not recommended.
Other reasons why an induction may not be recommended are if a mother has a primary genital herpes infection at the time of birth, or within six weeks of her due date. An induction is also not recommended if a woman has cancer of the cervix or any other contraindications to labour or vaginal birth.
How is labour induced?
Your doctor or midwife will do a vaginal examination and check your cervix. This procedure can be uncomfortable, but this will provide important information about how ready you are for labour and if your labour has started.
The most common ways to induce labour are:
- Membrane sweeping, also called a ‘stretch and sweep’ – is a procedure which happens during a vaginal examination. The maternity care provider feels for the amniotic sac or membranes and gently moves the membranes around the baby from the wall of the uterus.
- Breaking the waters. This is also called artificial rupture of the membranes or an ‘ARM’.
- Having an ARM and an intravenous drip which contains oxytocin – an artificial hormone which starts the uterus contracting.
- Prostaglandins – these are contained in a gel which helps the cervix to dilate.
- A balloon catheter – this is positioned inside the cervix and the balloon is inflated with saline/water.
Are there any risks to inducing labour?
The general agreement is that having an induction is a solution when there are risks in waiting until natural labour starts. However, there can also be some risks associated with an induction.
- Having a failed induction – this can happen when an induction is done but it doesn’t result in a vaginal birth and a caesarean section may be necessary.
- Lowered foetal heart rate.
- Infection – An ARM may increase the risk of infection for a mother and her baby.
- Uterine rupture – This can happen if the uterus tears along the scar line from a previous caesarean section.
- When an induction is done for reasons other than a prolonged pregnancy, it may increase the chance of needing a caesarean section.
- Women who are induced tend to experience more blood loss after birth.

Weighing up what’s right for you
Only you, your partner and your maternity care provider can know what is right for you. It’s easy to feel overwhelmed and unsure, especially when pregnant and it’s so important to make careful decisions. There are many factors to consider when deciding whether the benefits of having an induction outweigh the risks. Speak openly with your maternity care provider and let them know if you have any concerns.
You have agency over your body and it’s important you feel empowered and sufficiently informed to make decisions around what is right for you and your baby. Our online birthing course can provide helpful information to understand and take charge of your labour experience with modules covering delivery, postpartum care and more.
About the Author:
Written for Nourish Baby by Jane Barry. Jane has qualifications in general, paediatric, immunisation, midwifery and child health nursing. She holds a Bachelor Degree in Applied Science (Nursing) and has almost 35 years specialist experience in child health nursing. She is a member of a number of professionally affiliated organisations including AHPRA, The Australasian Medical Writer’s Association and Australian College of Children and Young People’s Nurses.
References
Induced labour | Pregnancy Birth and Baby (pregnancybirthbaby.org.au)
Inducing labor: When to wait, when to induce - Mayo Clinic
Induction of labour | The Royal Women's Hospital (thewomens.org.au)
Our Products
-

01. Guide to a Healthy Pregnancy
$55 -

02. Positive Birthing Course
$55 -

03. Infant Feeding Guide
$55 -

04. Baby Sleep Guide - First 12 Months
$55 -

05. Toddler Parenting Course 1 - 3 Years
$55
-
 When to Start Antenatal Classes?
When to Start Antenatal Classes?
Becoming a parent is an incredible milestone, but it comes with a host of changes that can be daunting, especially for first time parents. Antenatal classes are all about offering expectant parents the education they need to make informed decisions, look after their bodies and care for their newborn babies. While you probably already have a long list of things you need to accomplish during your pregnancy, it’s a good idea to make time to attend antenatal classes.
-
 Development Milestones 4-8 Months
Development Milestones 4-8 Months
As they reach the middle of their first year, you'll start to see bigger leaps in their growth and ability!
In this article, we’re going to discuss your baby’s developmental milestones between 4-8 months, and what you can expect along the way.





 When to Start Antenatal Classes?
When to Start Antenatal Classes?
 Development Milestones 4-8 Months
Development Milestones 4-8 Months








